Summary
Philadelphia struggles to meet the primary health care needs of its poor citizens. Over-utilization of emergency room services to treat nonurgent matters, because of reduced access to primary care, has escalated health care costs to unmanageable levels. Poor public health also negatively impacts the city’s educational system. Students with chronic conditions may disproportionately suffer from absenteeism and reduced academic performance, which can impact timely graduation. Philadelphia high school students are also unprepared for either the workforce or post-secondary opportunities. The Sayre Health Center, created through a partnership of the University of Pennsylvania, William L. Sayre High School, and the West Philadelphia community, provides a simple solution to multiple problems.
Sayre Health Center, housed within Sayre High School in the Cobbs Creek neighborhood of Philadelphia, is a 501(c)(3), school-based Federally Qualified Health Center (FQHC) that offers access to affordable health care, health education, and health literacy to community members. Through its innovative “Meds and Eds” program, the brainchild of co-founder the late Dr. Bernett L. Johnson, Jr., Sayre Health Center prepares Sayre High School students for careers in allied health fields. Undergraduate and graduate students from the University of Pennsylvania also experience service-based learning and interdisciplinary education at the Center. The cumulative effect on education is a continuum of mentorship from high school through to professional life.
By jointly addressing the health care and educational needs of its community, Sayre Health Center is uniquely positioned to offer social benefit. However, to maximize its impact, the Center should consider opportunities to expand, such as getting involved in day-to-day care for the Sayre High School student population. This recommendation, while not without possible difficulties, would reduce the burden on the school nurse, potentially reduce absenteeism, and have a net-zero impact on the school budget. This model could easily be replicated in other high schools.
Bernett L. Johnson, Jr., MD (1932-2009), received his medical degree from Meharry Medical College in 1957. Dr. Johnson had an illustrious clinical and military career. In the Navy, he achieved the rank of Captain and received the Legion of Merit for exceptionally meritorious conduct in the performance of outstanding services and achievements while serving as Commander of the Naval Hospital of Yokosuka, Japan. As a civilian, he was a Professor of Dermatology and Pathology at the University of Pennsylvania School of Medicine while serving in other major roles as the Chief Medical Officer of the Hospital of the University of Pennsylvania, Senior Associate Dean of Veterans Affairs, and the Senior Associate Dean for Diversity and Community Outreach. Dr. Johnson made indelible impressions on his students, his patients, and the staff of the University of Pennsylvania Medical School and Health System. Through his vision of the “Meds & Eds Service Model,” personal dedication, and team-building capabilities, the Sayre Health Center was opened in 2007. In honor of Dr. Johnson, the health center was renamed the Dr. Bernett L. Johnson Jr. Sayre Health Center on March 30, 2010.
Summary
Philadelphia struggles to meet the primary health care needs of its poor citizens. Over-utilization of emergency room services to treat nonurgent matters, because of reduced access to primary care, has escalated health care costs to unmanageable levels. Poor public health also negatively impacts the city’s educational system. Students with chronic conditions may disproportionately suffer from absenteeism and reduced academic performance, which can impact timely graduation. Philadelphia high school students are also unprepared for either the workforce or post-secondary opportunities. The Sayre Health Center, created through a partnership of the University of Pennsylvania, William L. Sayre High School, and the West Philadelphia community, provides a simple solution to multiple problems.
Sayre Health Center, housed within Sayre High School in the Cobbs Creek neighborhood of Philadelphia, is a 501(c)(3), school-based Federally Qualified Health Center (FQHC) that offers access to affordable health care, health education, and health literacy to community members. Through its innovative “Meds and Eds” program, the brainchild of co-founder the late Dr. Bernett L. Johnson, Jr., Sayre Health Center prepares Sayre High School students for careers in allied health fields. Undergraduate and graduate students from the University of Pennsylvania also experience service-based learning and interdisciplinary education at the Center. The cumulative effect on education is a continuum of mentorship from high school through to professional life.
By jointly addressing the health care and educational needs of its community, Sayre Health Center is uniquely positioned to offer social benefit. However, to maximize its impact, the Center should consider opportunities to expand, such as getting involved in day-to-day care for the Sayre High School student population. This recommendation, while not without possible difficulties, would reduce the burden on the school nurse, potentially reduce absenteeism, and have a net-zero impact on the school budget. This model could easily be replicated in other high schools.
Bernett L. Johnson, Jr., MD (1932-2009), received his medical degree from Meharry Medical College in 1957. Dr. Johnson had an illustrious clinical and military career. In the Navy, he achieved the rank of Captain and received the Legion of Merit for exceptionally meritorious conduct in the performance of outstanding services and achievements while serving as Commander of the Naval Hospital of Yokosuka, Japan. As a civilian, he was a Professor of Dermatology and Pathology at the University of Pennsylvania School of Medicine while serving in other major roles as the Chief Medical Officer of the Hospital of the University of Pennsylvania, Senior Associate Dean of Veterans Affairs, and the Senior Associate Dean for Diversity and Community Outreach. Dr. Johnson made indelible impressions on his students, his patients, and the staff of the University of Pennsylvania Medical School and Health System. Through his vision of the “Meds & Eds Service Model,” personal dedication, and team-building capabilities, the Sayre Health Center was opened in 2007. In honor of Dr. Johnson, the health center was renamed the Dr. Bernett L. Johnson Jr. Sayre Health Center on March 30, 2010.
Barriers to Health Care and Impact
Barriers to Health Care and Impact
Despite being home to four academic medical centers and hundreds of local private health care practices, Philadelphia struggles to meet the health care needs of its citizens. Philadelphia has the highest number of low birthweight babies, the highest infant mortality rate, and the lowest percentage of women receiving prenatal care relative to its four surrounding counties (Bucks, Chester, Delaware, and Montgomery) in Southeastern Pennsylvania. In addition, Philadelphia has a three-fold higher death rate for heart disease and HIV/AIDS than its neighbors (Community Health Database 2010).. Infant mortality rates and substandard immunization—potential surrogate measures for malnutrition and access to prenatal and early childhood care, respectively—are also typically high in low-income families.
Several of Philadelphia’s low-income neighborhoods are classified by the U.S. Department of Health and Human Services Health Resources and Services Administration (HRSA) as Health Professional Shortage Areas (HPSAs), Medically Underserved Areas (MUAs), and areas with Medically Underserved Populations (MUPs) (HRSA 2010). By definition, an HPSA has a shortage of primary medical, dental, or mental health providers. An MUA is usually geographically based but can include a population component, while MUPs are designated by the socioeconomic status of a population. The Cobbs Creek neighborhood in West Philadelphia where Sayre is located is designated as an HPSA because of its lack of primary care providers, and it is also an MUA/MUP.
One of the roles of primary care is to identify risk and prevent problems. The financial benefit of adequate primary care cannot be overestimated. Without primary care, problems drive patients to seek care at the nearest emergency room. ER visits in the United States escalated from 90.3 million in 1996 to 119 million in 2006 (a 32% increase), and hospital admissions from the ER rose 50 percent during that same period (Arvantes 2008). The data suggest that repeat hospital admissions and repeat ER visits could be avoided if these patients had adequate primary care (Agency for Healthcare Research and Quality 2010)..
For students attending William L. Sayre High School in Cobbs Creek, data suggest a prevalence of health problems consistent with groups lacking adequate primary care. Almost 25 percent of the children between the ages of 13 and 17 living in the zip codes surrounding Sayre have asthma, while 21 percent of these youth are in fair or poor overall health. Of the total number of youth within this age bracket who are uninsured, 20 percent are also in poor health. Nearly 18 percent of these youth labeled as poor have bad health overall, and the rate is as high as 16 percent among those not considered to be living in poverty. One of the most common contributors to chronic health problems is obesity and, notably, 67 percent of the children over the age of 6 in the Sayre High School catchment area are considered to be overweight or obese (Community Health Database 2010). Chronic health conditions have a secondary effect on student school attendance. Children with poorly controlled asthma miss an average of six days of school every six months, compared with about three missed school days for their peers with more effectively controlled asthma (Altru Health System 2008).. Students with poor attendance are at greater risk for dropping out of high school.
Philadelphia Students: Low Graduation Rates and Unemployable
Philadelphia Students: Low Graduation Rates and Unemployable
In Philadelphia over the past decade, the graduation rate for high school students has hovered between 50 and 60 percent. Half of the students that enter as freshman do not graduate within four years. Philadelphia lags far behind the Pennsylvania state average of 80 percent and the national average of 68 percent (Institute of Education Sciences 2008). Nearly twice as many African Americans drop out of high school as Caucasian students (CNN.com 2009). Around 80 percent of the students within the Philadelphia School District are minorities, 62 percent of whom are African American (School District of Philadelphia website n.d.). Students from low-income families are six times more likely to leave school than wealthier students. In Philadelphia, socio-economic factors compound the dropout problem. Many families live below the poverty line, with the median household income less than $37,000 annually (City-Data.com n.d.).
The National Dropout Prevention Center/Network reports that high school dropouts are more likely to apply for and receive public assistance than high school graduates. The average high school dropout earns $143 a week less than high school graduates. Difficulties making enough money to meet basic needs can lead to additional problems, such as trouble with the law. For example, 82 percent of prisoners in the United States are high school dropouts (National Dropout Prevention Center/Network n.d.).
Among the 40 percent of Philadelphia students who do graduate from high school, many still lack the skills to obtain and retain gainful employment. In a study of over 400 employers, high school graduates were deficient in basic reading, math, and written communication skills, as well as in less tangible skills employers wanted their workers to possess, such as critical thinking, professionalism, and work ethic (Barrington and Casner-Lotto 2006).
In another report, employers identified as the main reason for not hiring someone a lack of basic employable skills such as being on time, attendance, and work ethic (Barton 2006). Lack of work experience detracts from marketability as employees, contributing to the current 10.9 percent unemployment rate for high school graduates (Brubaker 2010). Of employed high school graduates, many are underemployed, with low-paying or part-time work. Underemployment and unemployment lead to dependence on public assistance programs to meet an individual’s basic needs.
The same skill deficits that interfere with employability also hinder a student’s ability to get into post-secondary schools and training programs. In 2002, only 23 percent of African American high school graduates left with the minimum skills and credentials required to enter a four-year college (Alliance for Excellent Education 2009). Only about 25 percent of high school juniors and seniors in Philadelphia take the SAT, a required aptitude exam for the majority of colleges (Davis 2004). Of the students that do take the SAT or ACT exams, a large proportion do not score high enough to meet the entrance requirements of many four-year universities. In addition, many students do not get the experiences that they need in high school—advanced courses or extracurricular activities—to be viable candidates for post-secondary options.
The School District of Philadelphia and individual schools have initiated various programs attempting to increase graduation rates and provide a brighter future for students. Programs beginning in elementary school are designed to keep kids on target with their academics, while many middle schools try to excite students about the possibility of going to college. In high schools there are programs for tutoring, mentoring, enrichment opportunities, after-school programs, SAT prep programs, and college and career readiness programs. These hundreds of programs are distributed among Philadelphia high schools and have varied success as measured by graduation rates.
There are also a number of vocational and training programs within schools attempting to address the need for a trained workforce upon graduation. The majority of these programs are structured so that students learn their vocation through an onsite classroom simulation. These scenarios provide students with opportunities to practice their skills, but often lack some of the real world components of the business. For example, a culinary school within a public high school may have an onsite student-run kitchen and restaurant where students are able to hone their skills and techniques by running a restaurant for the teachers of the school. In this instance, students are learning about working in a restaurant, but the entire staff is composed of their classmates, and their “boss” is their teacher.
To supplement this model of training, other programs enable students to perform internships off site in a professional business environment. However, these programs are not as common because many companies and organizations are hesitant to participate, concerned about limited cost-effectiveness, liability, and the general inefficiencies that go along with training someone versus hiring someone who is already job-ready.
The Solution: Sayre Health Center
The Solution: Sayre Health Center
Sayre Health Center, located in Sayre High School, is a 501(c)(3), school-based Federally Qualified Health Center (FQHC) that is a partnership between the University of Pennsylvania, the Sayre High School, and the West Philadelphia Community. Sayre Health Center provides access to affordable health care, health education, and health literacy to all members of the community. As an FQHC, Sayre provides primary care services for all age groups independent of an individual’s insurance status or ability to pay. FQHCs are designed to bring affordable care to the poor and are located within HPSAs, MUAs, and MUPs. FQHCs are sustainable because they receive operational funding under Section 330 of the Public Health Services Act and cost-based enhanced Medicare and Medicaid reimbursement.
Sayre Health Center, unlike other FQHCs or school-based health centers, also prepares high school students for careers in allied health fields through its “Meds & Eds” program. Sayre High School students enrolled in the internship program work at the Health Center under the supervision of clinical and administrative staff. Undergraduate and graduate students from the University of Pennsylvania experience service-based learning and interdisciplinary education at Sayre Health Center. Medical students and medical residents rotating through the Health Center serve the community and act as near-peer mentors to high school students and undergraduates alike. The unexpected links between health care, hands-on training, and mentorship make the Sayre Health Center an innovation worth replicating.
Sayre meets health care needs
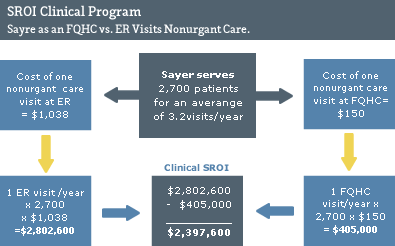
Since its doors opened in 2007, the Sayre Health Center practice has increased its service from a modest 370 patients in the first year to over 2,700 patients projected for 2010. Sayre patients visit the practice an average of 3.2 times per year (8,640 patient encounters for 2010). The cost of treating a nonurgent matter in an ER setting is higher than in a primary care setting. Average expenses for a visit to the ER were $1038 in 2007, according to the Medical Expenditure Panel Survey (Consumer Health Ratings.com n.d.). In contrast, the average cost of visiting a primary care physician (general practice, family medicine, internal medicine and pediatric physicians) in the United States is $100 based on fee-for-service (Agency for Healthcare Research and Quality 2007). The direct cost difference, on average, is $938.
Both Medicare and Medicaid reimburse FQHCs according to an all-inclusive per encounter calculation rather than on a fee-for-service basis. The Medicare All Inclusive Reimbursement Rate (AIRR) is nationally capped per visit at $112/encounter for urban FQHCs. The average FQHC Medicaid reimbursement is about $150 per patient encounter, but Medicaid reimbursement is state-regulated and clinic-specific. If all encounters at Sayre had been reimbursed at the $150/encounter Medicaid rate, then the total publicly funded healthcare expense for Sayre would have been $1.3 million. If the Sayre Health Center did not exist and each of Sayre’s patients had to go to the ER only one time during the year at $1,038/visit, the cost would be $2.8 million. The estimated savings, or Social Return on Investment (SROI), of an urban FQHC like Sayre is about $2.4 million for as few as 2,700 individuals.
Sayre meets educational needs
There is a need for educational programming that will keep students in school and on track to a successful career. Sayre Health Center meets this need through its dual mission to provide clinical care and educational opportunities for students. What sets this program apart from other high school training initiatives in Philadelphia is that it combines best practices from other schools by providing hands-on learning in an onsite professional environment. Student interns are not merely practicing their skills in a simulated scenario, but rather are experiencing working in a functioning health clinic with regular patients and operations without leaving their school grounds. The time commitment is also intensive, with interns working 10 hours per week during the school year and 20 hours per week during the summer months.
The intern program at Sayre is funded through the Philadelphia Youth Network and through the Public Health Management Corporation’s Out of School Time programs. Therefore, in addition to receiving invaluable experiences, students are able to receive minimum wage for their internships. This type of incentive can be very appealing to teenagers, particularly in difficult economic times when higher levels of unemployment for adults make it difficult for teenagers to get jobs.
Sayre Health Center interns receive hands-on training in the health center, learning skills such as recording patients’ vital signs, performing intake, and organizing outreach efforts. Throughout this process students are closely mentored by Sayre Health Center staff and are exposed to the variety of opportunities available to them in health care. To provide a holistic experience for the interns, they also participate in regular reflection activities and create projects that benefit individual and community goals. Past projects have included creating a Sayre Health Center brochure and creating a compilation of their experiences for the next class of interns. In addition, students are exposed to other enrichment and academic activities such as a summer book club in which the staff at Sayre and the students read a book and then meet to discuss it.
Interns also work at the grassroots level to improve health care access for their community through direct outreach. This type of work ties into Sayre’s goal to provide health education and literacy to the surrounding community. Examples of how students carry out this work include hosting family fitness nights and healthy cooking classes. To expand their work with Sayre students, Sayre Health Center is creating a Career and Technology Education class with a focus on allied health for high school juniors and seniors, which enables them to become Certified Medical Assistants at the end of the training. Ideally, this program would provide more opportunities for students to become involved and also to obtain much-needed job training.
An additional benefit to the educational mission is that, through its partnership with the University of Pennsylvania, Sayre Health Center has targeted undergraduate and graduate students as part of its program goals. The University of Pennsylvania School of Medicine sends two medical students each month for a four-week rotation at Sayre Health Center, giving their students local experience in an FQHC. Sayre Health Center also works with graduate-level social work, nursing, and dental students. Sayre incorporates undergraduate students from the University into their outreach and education efforts for the community and school by tapping into academically based community service courses at Penn that combine classroom lecture with hands-on community work. Through these programs, Sayre students have opportunities to interact with near-peer role models, while students from the University have the opportunity for experiential learning in the West Philadelphia community.
By observing university undergraduate and graduate students and with guidance from professional mentors, students from Sayre High School are positively impacted by the educational programs at the Sayre Health Center. Sayre Health Center employs two full-time physicians, nurses, medical assistants, and administrative staff who help to effectively train the student interns through hands-on experiences and coaching. In addition, one a staff member is solely dedicated to overseeing the educational components of the programming. This role provides additional one-on-one support that student interns may require throughout the program. Research reveals that high-quality interpersonal relationships positively contribute to students’ motivation, engagement. and achievement (Martin and Dowson 2009). As a result of Sayre’s intern program, students have a greater chance of graduating and being prepared for the job market than their peers who are not receiving this level of support. As a result, the graduation rate for students participating in this program could be calculated to be as high as 90 percent (not 100 percent because of accounting for external possibilities such as moving to another school). Therefore, over a five-year period, approximately 30 students will have participated in the internship program, of which we can assume that about 27 will complete the program and graduate high school on time.
Possibilities for the Future
Possibilities for the Future
Sayre Health Center is a Community Health Center that is located in a school, but it does not currently follow the School-Based Health Center (SBHC) model. There are 2,200 SBHCs in the United States providing preventative and primary care for the entire student population within a specific school.
According to the National Assembly of School-Based Health Centers (NASBHC, 2010), the SBHC model brings health care providers into schools to provide primary and preventative health care and avoid health-related absences. These centers are typically located in a school building, providing a comprehensive range of services and employing a multidisciplinary team (doctors, nurses, social workers, dentists, etc.). Clinical services are delivered by a qualified health provider, and the clinics require parents to provide written consent for their child to receive care. The health centers also function cooperatively with the school as an integral component, and they have a diverse advisory board that includes parents and the community (NASBHC 2010). Pennsylvania has only 28 SBHCs, a low number when compared to neighboring Maryland, which has 71, and New York, which has 206, and on the lower end overall when compared to all 50 states. In Philadelphia, a school district with around 300 schools and 170,000 students, there are fewer than five functioning SBHCs.
Unlike with a traditional SBHC, the students enrolled at Sayre High School do not automatically have access to the Sayre Health Center as their primary provider. Health care services for the student population during the school day are provided by the school nurse. Students at Sayre High School may, coincidentally, receive primary care services at the Sayre Health Center if they elect to do so, but there is no cross communication between the Health Center and the school nurse. In fact, if a student who happens to be a regular patient at the Health Center becomes sick during the school day and needs to be seen at the Health Center, that student must “sign out” of school, exit the building, walk around to the entrance to the Health Center, and reenter the building through the Health Center. A door connects the Health Center directly to the interior of the school, but it is not used.
What is clear from publicly accessible documents is that the school nurse is accountable for a wide range of responsibilities. The School District of Philadelphia School Nurse Policy Manual (School District of Philadelphia School Health Services 2002), Section 1402(a) of the School Code, requires periodic physical exams, vision and audiometric screening, and growth and scoliosis screening. In addition to these mandated program duties, the school nurse is charged with maintaining immunization records and testing for tuberculosis in collaboration with the City of Philadelphia Department of Public Health. The school nurse can be also be called upon to provide emergency care for students according to the plan, developed by the principal, for the care of ill or injured persons within the school. This plan includes an assumption of responsibility at the level of the school for the provision of immediate care, parent/guardian notification, disposition and/or transportation to home or hospital, and, when required, directing the parent/guardian to other sources for care. In this scenario, the ratio of students potentially needing care to nurses able to deliver care is clearly very high. The number and severity of triage events a nurse is required to manage can vary widely.
The logistics of absorbing the responsibilities of an SBHC at a location that is already serving the community at large may not be as straightforward as opening the intervening door. There are other things to consider, capacity being foremost among them. Discussions with the Medical Director of the Sayre Health Center, Kent Bream, MD, suggest that the Health Center does have adequate physician and non-physician staffing to accommodate the primary care needs of potentially 655 more patients. However, the potential increased patient load could be smaller depending on how many Sayre High School students are already current patients of the Health Center.
There is no way to know, from the Health Center’s point of view, how many students at Sayre High School are already patients at the Health Center, since there is no clinical cross talk between the Health Center and the school nurse. It is not standard practice to note the school of record in a patient’s medical chart. However, as previously mentioned, Sayre’s surrounding neighborhood has been classified as both an HPSA and an MUA/MUP. It is reasonable to assume that a sizable proportion of students who attend Sayre—which is not a magnet school and enrolls students from its vicinity —already get primary services from the Health Center. The potential added burden to the Health Center would then drop accordingly.
If the School District of Philadelphia engaged SBHCs, mechanisms to ensure the privacy of student-patients would have to be revisited. Another matter that cannot be ignored is whether it is appropriate and beneficial to the students to have both a complete academic record and a complete health record housed at the same facility. There are definite practical benefits to having a student’s primary care physician “in house.” Examples of chronic health conditions potentially faced by school nurses include asthma, diabetes, and allergies (National Association of School Nurses 2006). .Children with poorly controlled asthma miss an average of six days of school every six months, compared with about three missed school days for their peers with more effectively controlled asthma (Altru Health System 2008). Having a child’s primary care provider at school might help with reducing missed school days and improve educational outcomes. Early dismissal resulting from an asthma flare-up during the school day also negatively impacts working parents. If unplanned dismissals could be reduced, secondary consequences to the family, such as lost work time, could also be avoided.
Other states have successfully utilized SBHCs for nearly half a century. According to the National Association of School Nurses (NASN), school nursing has emerged as a specialized practice area of nursing that provides the “critical link between the education system, students, families, community, and medical care” (NASN 2001). In this same position statement, the NASN recognizes that increasing numbers of students require more complex care and that these students may not have access to appropriate health care. The final recommendation of the NASN is in support of a partnership between school nurses and SBHCs:
To facilitate optimum student health and educational outcomes, it is the position of the National Association of School Nurses that both school nursing services and SBHCs can provide unique and valuable services for children and youth. When available, school-based health centers should be integrated with school nursing services in a non-hierarchical and seamless partnership that provides health services in a confidential, safe, effective, and evidence-based system of care. This integration of school nursing services and the services of SBHC staff ensures that children and youth will have access to the health services they need and enhance the positive outcomes for the students (NASN 2001).
At the moment, with the Sayre Health Center in place for three years, the School District of Philadelphia is uniquely positioned to give the SBHC mechanism for student health management a “test drive” without sacrificing the current services of the existing school nurse. The Health Center is separately incorporated, locally staffed, federally funded, and operates in partnership with the University of Pennsylvania and the University of Pennsylvania School of Medicine. The SROI from the clinical services offered at Sayre has already been discussed.
A window of opportunity to replicate the physical space of Sayre Health Center at a second community high school at relatively low cost is closing. A new West Philadelphia High School building at 49th and Chestnut Streets is currently under construction. Modifications to accommodate a health center similar to Sayre would cost less if implemented now than if a health center were to be retrofitted after the close of construction. Lastly, Philadelphia is home to five major academic hospitals, all of which are conveniently located near at least as many high schools. Replicas of the Sayre-Penn-community triad could be developed city-wide if directed by a vision similar to that of Dr. Bernett Johnson and supported by engagement from the community and the City of Philadelphia.
Lamont Marshall, The first recipient of the Dr. Bernett L. Johnson, Jr. Scholarship.
Lamont Marshall is exemplary of everything that Dr. Bernett Johnson’s Meds & Eds Model of Social Innovation can accomplish. While Lamont attended Sayre High School, he and his family, as residents of the neighborhood, utilized the health center for clinical services. As a student, Lamont became intrigued by the student training program offered right under his school’s roof. Lamont had the desire to further his education but lacked sufficient support structure to carry his dreams further. Fortunately, in the spring of his senior year at Sayre, Lamont began an internship at the Health Center that continued after his June 2009 graduation through to August. In September of 2009 he joined the Health Center as a full-time employee. Lamont is still employed at the Health Center, attends Community College of Philadelphia as the first recipient of the Dr. Bernett L. Johnson, Jr. Education Scholarship, and plans to pursue veterinary studies. Lamont serves as a mentor to current students at Sayre High School and cites the internship program as critical to his success.
The degree to which additional financial benefit can be realized from expanding the role of the Sayre Health Center to include that of a SBHC depends on additional factors not directly accessible to the public (i.e., the number of students at Sayre who receive health care through Medicaid and the detailed costs to the School District of Philadelphia for emergent and chronic care provided by the school nurse). What qualifies the Sayre Health Center as a true innovation, worth of replicating, is the site-specific “Meds & Eds” model of mentorship that has the potential to transform the educational experience, from high school through medical residency, in a way not previously attempted.
Elizabeth Yackel received a BA from James Madison University and an MSW from SUNY Albany. She is an Associate Director of Civic House, the University of Pennsylvania’s center for student-led community service programs. Elizabeth is also pursuing a Certificate in Nonprofit Administration through the Fels Institute of Government at the University of Pennsylvania. Annamarie Horan earned a BS in Biology from St. Joseph’s University and a PhD in Pathology (Radiation Oncology) from the University of Pennsylvania. She is enrolled in the MGA Program at the Fells Institute of Government at the University of Pennsylvania and will graduate in May 2011. She is the Clinical Research Director for the Department of Orthopaedic Surgery at the University of Pennsylvania. She considers herself fortunate to have had the pleasure of meeting and interacting with Dr. Johnson.
References
References
Agency for Healthcare Research and Quality. (2007, April 25). Primary Care Doctors Account for Nearly Half of Physician Visits but Less Than One-Third of Expenses. AHRQ News and Numbers. Available at http://www.ahrq.gov/news/nn/nn042507.htm (accessed July 25, 2010).
Agency for Healthcare Research and Quality. (2010, May 16). One in Four Patients Experienced Revolving-Door Hospitalizations. Available at http://www.ahrq.gov/news/nn/nn052610.htm.
Alliance for Excellent Education (2009, December 17). Achievement Gaps. Available at http://www.all4ed.org/publication_material/AchievementGaps (accessed July 25, 2010).
Altru Health System. (2008, October 31). Asthma Control Affects Absentee Rates: Missed Medications Mean Kids Miss School, Adults Miss Work. Health Highlights, Asthma Center Feature Story. Available at http://www.altru.org/body.cfm?xyzpdqabc=0&id=6&action=detail&aeproductid=HealthvisionArticles&aearticleid=asthma/nov08ascMain (accessed July 25, 2010).
Arvantes, J. (2008, August 27). Emergency Room Visits Climb Amid Primary Care Shortages, Study Results Show. AAFP News Now. Available at http://www.aafp.org/online/en/home/publications/news/news-now/health-of-the-public/20080827er-visits.html (accessed June 25, 2010).
Barrington, L., and J. Casner-Lotto. (2006). Are They Really Ready To Work? Employers Perspectives on the Basic Knowledge and Applied Skills of New Entrants into the 21st Century U.S. Workforce. Partnership for 21st Century Skills. Available at http://www.p21.org/documents/FINAL_REPORT_PDF09-29-06.pdf.
Barton, P. (2006). High School Reform and Work: Facing Labor Market Realities. Available at http://www.ets.org/Media/Research/pdf/PICHSWORK.pdf.
Brubaker, H. (2010, June 9). As Education Level Rises, Unemployment Rate Falls. Philly.com Business. http://www.philly.com/philly/business/homepage/20100609_As_education_level_rises__unemployment_rate_falls.html (accessed July 12, 2010).
Centers for Disease Control and Prevention. (2010). http://www.cdc.gov (accessed June 2, 2010).
City-Data.com. (n.d.). Philadelphia, Pennsylvania. http://www.city-data.com/city/Philadelphia-Pennsylvania.html (accessed July 23, 2010).
CNN.com. (2009, May 5). “High School Dropout Crisis” Continues in U.S., Study Says. http://www.cnn.com/2009/US/05/05/dropout.rate.study/ (accessed July 26, 2010).
Community Health Database, Philadelphia Health Management Corporation. (2010). http://www.chdbdata.org/ (accessed June 10, 2010).
Consumer Health Ratings.com. (n.d.). Average Cost for Hospital ER Visit, 2007, MEPS. Emergency Room—Typical Average Cost of Hospital ED Visit 2007. http://www.consumerhealthratings.com/index.php?action=showSubCats&cat_id=274 (accessed July 25, 2010).
Davis, B. (2004, July). On the Ground, “Word Did Not Get Out” About District's New SAT Push. The Philadelphia Public School Notebook. Available at http://www.thenotebook.org/july-2004/041401/ground-word-did-not-get-out-about-districts-new-sat-push (accessed July 23, 2010).
HRSA (Health Resources and Services Administration), U.S. Department of Health and Human Services (2010). Shortage Designation: HPSAs, MUAs & MUPs. Available at http://bhpr.hrsa.gov/shortage/ (accessed July 25, 2010).
Institute of Education Sciences, National Center for Education Statistics, U.S. Department of Education (2008). Public School Graduates and Dropouts from the Common Core of Data: 2007-2008.
Martin, A.J., and M. Dowson. (2009). Interpersonal Relationships, Motivation, Engagement, and Achievement: Yields for Theory, Current Issues, and Educational Practice. Review of Educational Research, 79(1).
NASBC (National Assembly of School-Based Health Centers). (2010). About School-Based Health Care. Available at http://www.nasbhc.org/site/c.jsJPKWPFJrH/b.2554077/k.BEE7/Home.htm (accessed November 23, 2010).
NASN (National Association of School Nurses). (2006). Position Statement: School Nursing Management of Students with Chronic Health Conditions. Available at http://www.nasn.org/Default.aspx?tabid=351 (accessed July 25, 2010).
NASN (National Association of School Nurses). (2001). Position Statement: The Role of the School Nurse in School Based Health Centers. Available at http://www.nasn.org/Default.aspx?tabid=245 (accessed July 25, 2010).
National Dropout Prevention Center/Network, Clemson University. (n.d.). Top 5 Reasons to Stay in School. Available at http://www.dropoutprevention.org/resource/family_student/reasons.htm (accessed August 6, 2010).
School District of Philadelphia School Health Services. (2002). School Nurse Procedure Manual. Available from: http://www.phila.k12.pa.us/offices/health/nurse_manual.pdf.
School District of Philadelphia website. (n.d.). About Us. Available at http://www.phila.k12.pa.us/about/ (accessed November 23, 2010).


