Access to oral healthcare is critical to overall health and remains a challenge, especially for low-income and vulnerable populations. In fact, there is a silent epidemic of oral diseases that is plaguing undeserved communities and without an innovative systems framework for improving oral health, the challenges will continue to be a barrier to a healthier population.
The national agenda for creating a healthier people has been set for decades. The Healthy People 2020 document and its stated goals for specific disease areas was set in motion by former U. S. Surgeon General, Dr. Julius Richmond, and his colleagues to set measures for increasing the human capital of the United States through the well-being of its citizens. With credit for the earliest public health innovation in the United States given to Paul Revere, we continue to strive toward the value proposition of health for all people. The nation is currently focused on a specific set of goals as stated in Healthy People 2020.
On the pathway to overall health and wellness, practices of healing and medicine have tracked human history with various and tremendous levels of advancement. Throughout this evolution, there has remained a difference between care focused on the individual and approaches that are required when poor health or illness affects a population. Innovative solutions in medicine become more relevant and necessary when diseases such as cholera, whooping cough, and more recently, HIV/AIDS, stymie the experts and ”downstream” medical interventions are the focus, treating symptoms to alleviate immediate suffering.
Urgency to save entire communities has forced innovation and dissemination (i.e., ”spread” not only for curative solutions and, more importantly, for generalizable preventive techniques). Prevention theories have led to the appreciation that community-wide solutions can mitigate the resource problems of a healthcare system focused on symptoms by better understanding the factors that contribute to better health. A 2003 National Call to Action to Promote Oral Health by the U.S. Surgeon General indicated that the nation could address the silent epidemic of oral diseases by applying similar theories.
One can look back to the health insurance experiments of the 1960s where innovations in reimbursement of healthcare providers for well-being rather than health impairment emphasized the value on prevention. A new resource distribution method was introduced with the hope of driving healthcare providers and patients toward a more effective and efficient system to maintain health. Those systems continue to be complex and misunderstood by patient and doctor alike. Similar thinking was applied to the maintenance of oral health, however a different financing system was created alongside employer-based medical coverage. A major difference of the dental financing system design is that it would not and, in many instances, still does not cover catastrophic events, but instead provides benefits in a prepayment model that can be applied to care expenses based on a set of standardized protocols.
The drivers for oral health and overall health are similar, the advances in science and opportunities for prevention align, however, the systems of care delivery and financing remain separate. Little change in the standardized protocols of oral care by dental professionals has been seen. Downstream treatments, identified in oral healthcare as restorations, are delivered mainly by surgeons who are situated in expensive suites where they repair broken enamel, root out damaging and painful nerve damage, and if needed, perform surgeries to diminish further pain and suffering. Advances in the field include new knowledge about the diseases of the mouth, their connections to systemic health, the complexity of the causal agents and conditions that promote disease progression, and more recently, how to assess individual disease risk. Still, prevention techniques to reduce oral diseases are mainly remanded to the interaction between the clinician and the patient at a time when the patient is more than likely facing consequences of oral diseases and in the context of how to stop them from getting worse. For the average person, the connection to and advice on prevention of oral diseases has come from manufacturers and distributors of chemicals that when applied by the user, can stop cavities, will refresh breath and create whiter teeth. Whether by clinician direction or marketed self-care methods, the mouth has been isolated from the rest of the body.
While the core principles of how to create better oral health are all in place, many people continue to face obstacles toward attaining oral health in the first place. Add to that the confusion about how the payment system is supposed to work, and the system-based obstacles increase. The working systems support an individual in need of repair, who can afford the help, and with a clinician who is well paid for their services. However, when measured against what is known through scientific, evidence-based and community-based research, the current systems fail to achieve to reach and/or provide quality care to millions of people. The field of oral health presents tremendous opportunities for systems transformation through innovative redesign of the way care is delivered, what it is designed to do, where it takes place, how it is paid for, who pays for it and what outcomes it produces. In order to address the burden of oral diseases carried by millions of marginalized people, existing systems call for disruption.
Disruptive innovation, introduced by Clay Christensen, is beginning to gain interest among oral healthcare providers. Primary care has embraced the innovation momentum for decades. The Quality Movement has been testing healthcare professionals and organizations for their effectiveness and efficiencies to reduce pain and suffering and to save lives. Public policy is driving Triple Aim expectations for appropriate reimbursement models not only for medicine, but with some degree of innovation, for oral healthcare services. Amidst these demands, the same primary actors are responsible for creating a nation of healthy people. The polarities of those humanitarian intentions are stark, when one considers that the systems within which these expectations are to be met are not designed to achieve those desired outcomes or to benefit all people. A systems view, with opportunities for innovation, is promising for redesign in consideration of the demand for new ideas, swift application, lower per capita costs and broader community engagement.
A systems approach becomes more useful in appreciation of what actually creates health and well-being. For decades, it has been understood that the major factors which impact health are those of environment, lifestyle, biological and genetic factors. This accepted view provides a broader framework within which resource allocation for healthcare can be more responsible and responsive. The health sector can then be effectively understood as part of a vast ecosystem of economic, social and cultural components that are unavoidably connected and interdependent as factors in creating its intended results.
As a function within the health sector, philanthropy is prone to directing funds to address immediate community needs, rather than investing at a larger systems level. In oral health, funding initiatives like Mission of Mercy provide necessary interventions as expressions of charity that, without their existence, would leave many people without any option for care. As a marginalized health problem for marginalized populations, oral diseases perpetuate health disparities and thus require social and systemic disruptive innovations to avoid conditions where the needs are dire and intervention measures are drastic. Oral health philanthropy has embraced opportunities to address these systems and promote the ideal states in the realms of policy, financing, care and community. The DentaQuest Foundation and its supporting enterprise have put forth a systems change framework that identifies the characteristics of the ideal states of these four systems. The theory of change to attain these ideal states requires the engagement of a broad and diverse network of stakeholders.
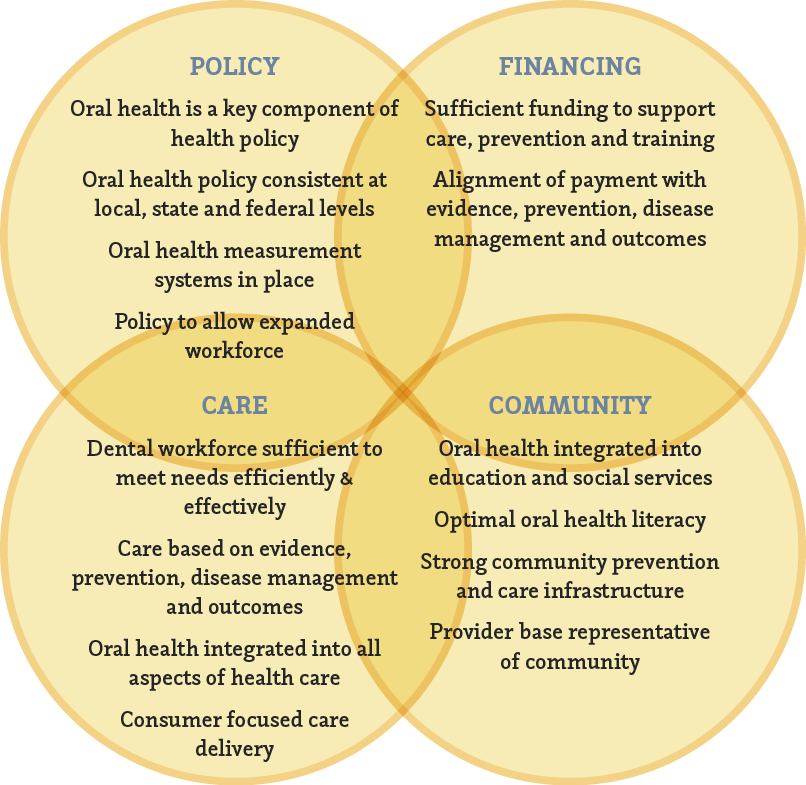
Figure 1: Systems Framework for Oral Health: The Ideal States of Policy, Financing, Care and Community.
Across the nation, a network of such stakeholders is moving the system components in consideration of their own place(s) and role(s) in the previously referenced ecosystem. Innovative champions from among the health professions are proving to be the primary change agents toward the attainment of the Care System component identified in the Figure 1 as: “Oral Health is integrated into all aspects of healthcare .”
To attain this population-oriented and person-centered improvement, a funding collaborative is supporting a systems solution that incorporates the mouth with the rest of the body. The National Interprofessional Initiative on Oral Health (NIIOH) is a co-funded network comprised of practitioners and experts from a range of health disciplines, including physicians, nurses and nurse practitioners, physician assistants, health professions educators and others who believe that oral disease can be eradicated, and are aligned in their efforts to integrate oral health into person-centered care as a solution. Previous to the development of NIIOH, primary care clinicians were more likely to omit mention or examination of the gums and teeth in the patient encounter, providing limited opportunity to identify abnormalities or to address early signs of disease.
This collaborative has revolutionized models for person-centered care that include oral health by developing Smiles for Life, a nationally-adopted oral health integration curriculum (Society of Teachers of Family Medicine 2016), influencing approaches to health professions education (Dolce, Holloman, and Fauteux 2016) and reforming clinical practices (Haber et al. 2015), (Hummel et al. 2015).
The integration of oral health into primary care is a systems-focused approach whose success, as it continues to spread, will improve patient health outcomes and has the vast potential to positively impact the populations of underserved and vulnerable communities. Multiyear evaluation of NIIOH strategies have revealed changes in practice, expanded and revised medical education curricula and professional collaborations on many levels.
These innovative solutions will continue to emerge through collaborative investments by funders and the network mindset of interdisciplinary champions. As we witness the early successes in interprofessional education, practice and financing innovations, it is likely that through the shift toward the priority of prevention, a fidelity to attaining the highest quality measures of individual and community life, and more equitable application of human and financial resources, will create a much healthier nation.


