Summary
Tooth decay is the single most common chronic childhood disease. Pediatric dental decay can result in an underweight child whose early growth and development are delayed. Pain from dental disease often causes reduced food intake because eating is painful. Remedial dental treatment in children has been proven to promote healthy weight gain, less pain and improved abilities to eat and sleep. Good pediatric dental hygiene is the start of a lifetime of good dental health and can make an indelible impact on the social and physical development of a young child.
Philadelphia’s children suffer from a lack of adequate pediatric dental care. This lack is compounded by the impact of the 35 percent of Philadelphia children who live below the poverty line. The problem is concentrated in North Philadelphia, where two of the city’s four Dental Health Professional Shortage Areas are located.
St. Christopher’s Foundation for Children is a public, grant-making charity that supports the health and well-being of children in the community served by St. Christopher’s Hospital for Children through programs in the areas of care, outreach, research and education. The Foundation has become a part of the pediatric dentistry solution in North Philadelphia. The Foundation’s leaders, recognizing the value of serving children in their own communities, introduced the Ronald McDonald Care Mobile in 2005. The Care Mobile offers comprehensive and continuous dental treatment at no cost to unserved and underserved young children. It has served over 5,000 new patients between 2005 and 2009, with services valued at over $1.25 million.
Meet Marcus
Four-year-old Marcus was in the North Philadelphia Head Start program, but his caregivers noticed that he never spoke, did not play with other children and was underweight. When asked, his mother attributed his behavior to his “shy” personality. However, his caregivers knew that something was wrong. The staff at Head Start, as well as Marcus’s mother, would come to learn that the boy was suffering from no less than 13 decaying teeth.
Summary
Tooth decay is the single most common chronic childhood disease. Pediatric dental decay can result in an underweight child whose early growth and development are delayed. Pain from dental disease often causes reduced food intake because eating is painful. Remedial dental treatment in children has been proven to promote healthy weight gain, less pain and improved abilities to eat and sleep. Good pediatric dental hygiene is the start of a lifetime of good dental health and can make an indelible impact on the social and physical development of a young child.
Philadelphia’s children suffer from a lack of adequate pediatric dental care. This lack is compounded by the impact of the 35 percent of Philadelphia children who live below the poverty line. The problem is concentrated in North Philadelphia, where two of the city’s four Dental Health Professional Shortage Areas are located.
St. Christopher’s Foundation for Children is a public, grant-making charity that supports the health and well-being of children in the community served by St. Christopher’s Hospital for Children through programs in the areas of care, outreach, research and education. The Foundation has become a part of the pediatric dentistry solution in North Philadelphia. The Foundation’s leaders, recognizing the value of serving children in their own communities, introduced the Ronald McDonald Care Mobile in 2005. The Care Mobile offers comprehensive and continuous dental treatment at no cost to unserved and underserved young children. It has served over 5,000 new patients between 2005 and 2009, with services valued at over $1.25 million.
Meet Marcus
Four-year-old Marcus was in the North Philadelphia Head Start program, but his caregivers noticed that he never spoke, did not play with other children and was underweight. When asked, his mother attributed his behavior to his “shy” personality. However, his caregivers knew that something was wrong. The staff at Head Start, as well as Marcus’s mother, would come to learn that the boy was suffering from no less than 13 decaying teeth.
The Problem: Lack of Pediatric Dental Care for Poor Children
The Problem: Lack of Pediatric Dental Care for Poor Children
The Surgeon General’s report on oral health care in America stated that “tooth decay is the single most common chronic childhood disease—5 times more common than asthma and 7 times more common than hay fever” (U.S. Department of Health and Human Services 2000). Yet, in a society in which dental care is sometimes thought to revolve around cosmetic veneers, implants and bleaching techniques, it may be difficult for us to fully appreciate the significant impact that a lack of pediatric dental care can have on a child. Even in mainstream pediatrics, the urgency of many dental problems is not immediately perceived, and so the impact of dental health on overall well-being is often overlooked in the context of more serious medical conditions (Reisine 1988). However, untreated dental bacterial decay, and the associated discomfort and toothache, lead to a failure to thrive in otherwise healthy children.
Tooth decay can be prevented by a combination of community, professional and individual measures, including water fluoridation, professionally applied topical fluorides and dental sealants, and the use of fluoride toothpastes. Yet tooth decay is the most common chronic disease of childhood. Dental care is the most prevalent unmet health need in children in the United States, with wide disparities existing in oral health and access to care. Almost three times as many children lack dental insurance as lack medical insurance. But the presence of third-party dental coverage does not reliably predict access to care. Children from poor families who qualify for Medicaid are entitled to comprehensive oral health coverage through the program's Early Periodic Screening, Diagnostic, and Treatment benefit. But despite this benefit, these children are less likely to receive dental care than children from middle- and upper-income families, many of whom lack dental coverage (Mouradian, Wehr, and Crall 2000).
Consequences of Pediatric Dental Decay
Consequences of Pediatric Dental Decay
Pediatric dental decay can result in an underweight child whose early growth and development are delayed. Pain from dental disease often causes reduced food intake because eating is painful. The child’s quality of life is also negatively impacted because of irritability and disturbed sleep habits, factors that inhibit growth in young children (Sheiham 2006). In infants, dental decay can destroy newly emerging teeth. These teeth are vital to proper nutrition and speech development, and they set the stage for future dental health (Pew Center on the States 2010a).
Cavities, abscesses and toothaches often lead to restricted activity at school, chronic school absence, and a diminished ability to focus in class and learn (Sheiham 2006). In 2000 the U.S. Surgeon General stated that in a single year, more than 51 million hours of school may be missed because of dental-related illness. These school absences contribute to a widening achievement gap, making it difficult for children with chronic toothaches to keep up with their peers academically (Pew Center on the States 2010a).
Untreated dental disease also impacts the national economy; taxpayers spend more to provide emergency care when dental disease becomes unbearable. Poor pediatric dental care also impacts the economy because parents have to take time from work to bring in their children for treatment (Sheiham 2006). Investing in pediatric dental care will alleviate obstacles to gainful employment for these children as they grow into adults; about 164 million work hours are lost each year in the United States because of dental disease. Dental problems can also hinder a person’s ability to secure a job, so the benefits of early investment in dental care result in a significant payoff to society (Pew Center on the States 2010a).
Lastly, dental disease leads to higher incidences of hospitalization and emergency dental visits. Increasingly, research points to the link between gum disease and cardiovascular disease, diabetes and stroke. The long-term results of dental disease can sometimes be even more severe. In 2007, a 12-year-old in Maryland and a 6-year-old Mississippi boy died because of severe tooth infections. Both were eligible for Medicaid but did not receive the dental care they needed. Unfortunately, it is unclear how many children suffer a similar fate, because official causes of death are usually identified as the related condition—for example, a brain infection—instead of the underlying dental disease (Pew Center on the States 2010a).
According to a 2007 Centers for Disease Control and Prevention study, the proportion of children between two and five years old who have cavities actually increased by 15 percent in the last decade. The same study found that poor children continue to suffer the most from dental decay. Children aged 2 to 11 whose families live below the poverty line are twice as likely to suffer from untreated decay as their more affluent peers. While 58 percent of children who have private insurance receive dental care across Pennsylvania, only 38.1 percent of their peers on Medicaid get dental care nationwide (Pew Center on the States 2010a).
The American Academy of Pediatrics’ journal states that children from poor and near-poor families (200% below the federal poverty level) are three times as likely to have an unmet dental care need as children from families with incomes 200 percent above the poverty line. Poor and minority children are also less likely to have dental visits. A 1996 Department of Health and Human Services inspector general's report noted that, in 1993, fewer than 20 percent of children enrolled in Medicaid, who were eligible for early screening benefits, received any preventive dental visits (Mouradian, Wehr, and Crall 2000).
Dental Care in Philadelphia
Dental Care in Philadelphia
In Pennsylvania, 28 percent of children are enrolled in Medicaid, but only 32 percent of those children received dental care in 2007 (Children’s Hospital of Philadelphia 2010; Pew Center on the States 2010b). The low socioeconomic status of many of Philadelphia’s children, 35 percent of whom live below the poverty line, compounds already inadequate pediatric dental care (City-Data.com 2007). While Philadelphia is home to many dental care providers, they often make appointments 90 to 100 days in advance, a schedule that is challenging for transient, low-income families.
Two of the city’s four Dental Health Professional Shortage Areas (DHPSAs) are located in North Philadelphia. The DHPSA classification means that the region is federally designated as having a shortage of dental care providers who accept Medicaid. The dentists that do take Medicaid and practice in this low-income area are often dental residents who leave after their training is complete. A 2008 Household Health Survey revealed that 23.3 percent of children in the six zip codes that make up North Philadelphia do not have access to dental care. The survey also demonstrated that the lack of dental care in North Philadelphia is more pronounced among racial minority and poor children: while all white children surveyed have some form of access to dental care, 25.8 percent of black children and 17.2 percent of Latino children do not. Thirty-two percent of poor children also lack access (Pennsylvania Health Management Corporation 2008). Dental practitioners note that self-reported survey data on dental care tends to be skewed conservatively. Many parents will not admit that their children do not get dental care, while others may erroneously count cursory dental screenings at health fairs or schools as preventive dental visits. In reality, the lack of pediatric dental care availability or uptake in North Philadelphia may be even greater than is currently estimated.
The Solution: Bringing Preventive Pediatric Dental Care to Children in North Philadelphia
The Solution: Bringing Preventive Pediatric Dental Care to Children in North Philadelphia
Remedial dental treatment in children has been proven to promote healthy weight gain, lessen pain, and improve eating and sleeping patterns. Pediatric dental care also has significant positive psychological and social effects on children. In one study, parents reported more smiling, improved academic performance and increased social interaction after their children received proper dental treatment (Sheiham 2006).
St. Christopher’s Foundation for Children is a public, grant-making charity that supports the health and well-being of children in the community served by St. Christopher’s Hospital for Children through programs in the areas of care, outreach, research and education. The Foundation has become a part of the pediatric dentistry solution in North Philadelphia, supporting a wide-ranging pediatric dental health program, including the Ronald McDonald Care Mobile, a mobile dental office owned by the Foundation, which offers access to comprehensive and continuous dental treatment at no cost to unserved and underserved young children. The program is primarily school-linked, serving over 70 area public, charter and parochial schools and pre-school programs. It also serves summer camps, a juvenile detention home, and shelters for homeless families. Nurses, social workers and child advocates at these partnering sites help to identify the children who desperately need dental care.
The Foundation’s dental program was introduced in 2005 and has since served over 5,000 new patients. The total value of the services provided between 2005 and 2009 is over $1.25 million. While insurance companies reimburse the Foundation for a portion of the services rendered, the actual cost is significantly higher. The Foundation partners with numerous entities to help offset these costs and maintain a high standard of care. The dental program is a vital one: young clients come to their first dental exam with almost double the decay rate reported as average for the nation, the state and the City of Philadelphia. About 43 percent of three-year-olds have one or more teeth with untreated decay; among eight-year-olds, about 72 percent have decay. Over 13 percent of the six-year-old clients who have their adult teeth have some form of decay at their first examination (St. Christopher’s Foundation for Children 2010).
Many of the young clients treated by the Care Mobile have recently emigrated from countries without fluoridated water or access to dental care. The families of these children may avoid drinking Philadelphia’s fluoridated water because they distrust public water based on their prior experiences. Many of these families will direct their childcare facilities to give their children only bottled water. Because baby teeth fall out, those with low health literacy are prone to underestimating or failing to recognize the importance of pediatric dental care. In addition, many low-income families do not have dental care for the adults in the household, and primary caregivers are “passing on” high bacterial loads to their children in addition to poor hygiene and nutrition habits.
How the Care Mobile Works
The Care Mobile is a 40-foot-long trailer that parks at the program’s various partner sites in North Philadelphia. The trailer, originally used for cursory medical checkups at health fairs, was retrofitted in 2005 as a dental office on wheels, fully staffed and available five days a week for children and their families. The national Ronald McDonald House Charities purchased the vehicle, donated it to the Foundation in partnership, and the Ronald McDonald Care Mobile was officially born. Long-term partners in the Care Mobile initiative include Ronald McDonald House Charities of the Philadelphia region, the Philadelphia Health Care Trust, and St. Christopher’s Children’s Hospital. Credentialed staff work full time, five days a week, supported by four pediatric dental residents; 24 pediatric medical residents and 26 senior dental hygiene students rotate in staffing the truck, receiving clinical experience in a public health setting. Hiring full-time staff is unusual for a community program like the Care Mobile, but these staff members are critical to ensuring the high consistency of care offered.
The real value of the Care Mobile is the ability to reach children in their own communities. As a staff member has attested, receiving an unfamiliar, sometimes painful treatment for a dental problem can be very intimidating to a frightened youngster. When children are treated in the shadow of their schools, or at their familiar Head Start program under the watchful eye of trusted adults, the experience tends to be less traumatic. The Care Mobile team becomes familiar to the families and childcare providers they interact with. The increased comfort level in the community enhances the likelihood that parents will follow up for future treatment for their children. Familiarity with the neighborhoods and the families also has helped the Care Mobile team to connect client who are experiencing non-health-related challenges to the appropriate community resources.
Value-Added of the Community Oral Health Initiative
Dr. Augustine Chialastri, the Dental Director of the St. Christopher’s Children’s Hospital and a long-time ambassador for pediatric dental care in Philadelphia, notes that preventive dental treatment is only as good as the instructions youngsters follow at home. Indeed, Dr. Chialastri’s commitment to holistic dental treatment led him to voluntarily oversee the Foundation’s dental program. As the program director for the residency program, he has his students make rotations in public health settings like the Care Mobile three times per week. The Care Mobile staff also recognizes the need for a holistic approach to dental care, as their program is just one of five components that make up the Foundation’s Community Oral Health Initiative.
The Community Oral Health Initiative improves the oral health of children and families in North Philadelphia through community awareness and partnerships, education, early intervention and treatment. “My Baby’s Smile” emphasizes prevention and offers information and therapeutic hygiene treatment to pregnant women. Parents are taught the basic visual cues that indicate severe dental damage. “My Marvelous Mouth” stresses education and delivers age-appropriate oral health information, integrated into the curricula of partner schools. This program was used in 24 partner schools in the 2009 fiscal year, providing child-friendly dental instruction to 4,178 children in kindergarten, third grade and seventh grade. “Diamonds and Pearls” focuses on awareness and distributes oral health information to adults in the Philadelphia region. This program aims to give adults a relatable metaphor for the value of their teeth, while teaching them to be smart consumers who make good oral health choices. The curriculum poses the question: How many of you have $120,000 in cash? Adults are then educated about how their teeth are in fact worth $120,000, and the value of good dentistry is explained.
As Julianna Gelinas, Director of Community Oral Health Initiatives at the Foundation, notes, “to tell a kid to ‘brush everyday’ is useless if they don’t have a toothbrush at home.” To remedy this problem, each patient at the Care Mobile gets a toothbrush and toothpaste, and is also given a toothbrush and toothpaste for each member of their household. Children receive colorfully illustrated workbooks created by the Department of Health, available in English and Spanish, which help to keep children’s attention while still offering an education, perhaps to their parents as well. Each child also gets floss, pamphlets and a pictorial instruction sheet on dental care.
The Care Mobile’s Social Return on Investment
Children are eligible to enter the Care Mobile program up through the third grade and are offered comprehensive and continuous care until age 17 if they have successfully kept up with annual preventive visits. The average cost to treat one uninsured child is $366 (St. Christopher’s Foundation for Children 2010). By comparison, to treat and operate on an uninsured four-year-old with severely decayed teeth costs the St. Christopher’s Children Hospital an astounding $26,955.1 Of the 1,702 new patients the Care Mobile treated in fiscal year 2009, at least 30 percent (or 510) had five or more cavities at their first exam (St. Christopher’s Foundation for Children 2010). Without early intervention from the Care Mobile, these 510 children are likely to have needed operatory care, which would have reached a total cost of $13,747,050. Instead, the Care Mobile treated them for a fraction of that potential cost: $186,660. Thus, the cost-savings is, conservatively, $13,560,390.
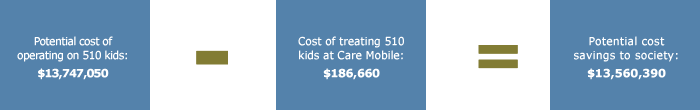
- ^Quote for operational care obtained from St. Christopher’s Children Hospital, based on treating a four-year-old in August 2009 who required dental treatment on 12 teeth with severe decay, at a cost of $1,429. Costs of operating on the child were an additional $25,526.16 for time in the operating room, general anesthesia and time in the recovery room.
The Foundation’s Plans for the Future
The Foundation’s Plans for the Future
Paul DiLorenzo, the Foundation’s Board President, is quick to acknowledge that while the Care Mobile model has been an uncontested success, the need for that particular service is tied to an even bigger, more complicated issue: a critical lack of pediatric dental care in Philadelphia. In an effort to increase access to dental care, Public Citizens for Children and Youth has collated a 32-page directory of resources for parents entitled Where to Go for Help: Oral Health Resources for Children & Adolescents (available at www.pccy.org). Jan Shaeffer, the Foundation’s Executive Director, notes that there are still many barriers to accessing information. Parents in North Philadelphia, who need the services the most, often don’t have the time to call all of the city clinics to find an available provider. The City of Philadelphia is constantly working to provide for the daunting number of parents who need their services but, because of a shortage of resources, the need remains great.
To complement the work of the directory, the Foundation also devotes resources to the preventive aspects of pediatric dental care. Accessible oral health education is a key part of their strategy. For example, the Foundation emphasizes to patients that you can catch germs from decay the same way you catch germs from a cold. Expectant mothers are also educated about dental care so that they do not risk infecting their children with the bacteria that causes cavities at an early age.. Prenatal dental care is gaining attention, as researchers continue to investigate links between the risk of preterm, low-birth-weight babies and periodontal disease.
The Foundation also wants to educate local pediatricians about their critical role in preventing irreversible dental damage. As Shaeffer explains, the staff of the Care Mobile “is seeing kids at three, four, and five years old, but many kids are already past the point of acceptable dental care.” Thus, the Foundation wants to raise awareness among North Philadelphia physicians so that they start looking into infants’ mouths starting at birth. The Foundation promotes the concept of the pediatrician’s office being a comprehensive “health home,” so that physicians, who see children at an earlier stage than most dentists do, will take the time to refer a child to the dentist. The American Medical Association notes that many professional associations now advise that children have dental assessment by age one to catch rampant early childhood infections, such as baby-bottle tooth decay, that are associated with inappropriate feeding practices. As the Association states, the decay process “is amenable to medical management before it results in frank cavities and before many children see a dentist” (Mouradian, Wehr, and Crall 2000: 2626).
As medical practitioners consider the implications of the newly passed federal health care reform legislation, members of the dental community are discussing the long-term ramifications for their field. The chair of the department of pediatric dentistry at New York University’s College of Dentistry celebrated the fact that, even as the bills were revised repeatedly, some support for children’s oral health was retained (Marcy 2009). However, the vice president of public and government affairs for a prominent insurance company expressed fear that such coverage will cause parents to drop their private insurance coverage, because their children will be included within the government’s care mandates (Marcy 2009). The American Dental Association opposed the proposed legislation, believing it ignored the need to expand benefits offered under Medicaid, which could potentially expand the treatment that many adults receive (Worldental.org 2010). Another long-term question that the Foundation asks is, if children get additional insurance in DHPSA areas, will there be an adequate supply of dentists to satisfy the demand? Insurance coverage only goes so far if there are not enough providers to meet patient demand. Hopefully the dental community will keep these issues at the forefront of the health care debate.
Marcus After the Care Mobile
Marcus After the Care Mobile
The Health Director of the North Philadelphia Head Start program referred four-year-old Marcus to the Ronald McDonald Care Mobile, and on May 27, 2009, the dentists extracted four of his upper teeth and treated the remaining 13 decayed teeth. To the delight of Marcus’s mother and the Head Start staff, changes in Marcus’s demeanor and physical well-being were immediate. Since he was in less pain, he regained his appetite and began to gain weight, and now he plays and talks all the time. The Director marveled at how proper dental care effectively alleviated his constant tooth pain, as well as his shyness and socialization. In September of that year, Marcus’s mother reached out to the staff of the Care Mobile, commenting, “I had just started a new job and couldn’t get a day off to take him to the dentist. I think [the Care Mobile] is a wonderful thing!” The Head Start teacher also wrote that, the day after Marcus’s second visit to the truck, “[Marcus] not only smiled at me for the first time, but I was actually able to understand the words he was trying to say. The Ronald McDonald Mobile gave this child a bright start and did wonders for his self esteem.” The impact of good pediatric dental hygiene cannot be underestimated—not only is it the start of a lifetime of good dental health, but it can make an indelible impact on the social and physical development of a young child.
Mikaela Levons has worked in the nonprofit sector for the past five years. She graduated from Princeton University with a Bachelor of Arts degree from the Woodrow Wilson School of Policy & International Affairs. She is currently a candidate for the M.Sc. in Nonprofit/NGO Leadership at the University of Pennsylvania. She is also a recipient of a Goldring Fellowship for Social Change.
References
References
Children’s Hospital of Philadelphia. (2010). Medicaid 101. Available at http://www.chop.edu/about/chop-in-the-community/government-affairs/medicaid-and-childrens-hospital.html (accessed March 5, 2010).
City-Data.com. (2007). Philadelphia, Pennsylvania (PA) Poverty Rate Data — Information About Poor and Low Income residents. Available at http://www.city-data.com/poverty/poverty-Philadelphia-Pennsylvania.html (accessed March 5, 2010).
Marcy, J. (2009, October 14). Health Bills Agree on Enhancing Kid's [sic] Dental Care. National Public Radio. Available at http://www.npr.org/templates/story/story.php?storyId=113792939 (accessed April 13, 2010).
Mouradian, W. E., E. Wehr, and J. J. Crall. (2000). Disparities in Children's Oral Health and Access to Dental care. JAMA , 284 (20): 2625–2631.
Pew Center on the States. (2010a, February). The Cost of Delay: State Dental Policies Fail One in Five Children. State Fact Sheets—Pennsylvania. Available at http://www.pewcenteronthestates.org/uploadedFiles/wwwpewcenteronthestatesorg/Initiatives/Childrens_Dental_Health/011_10_DENT%20Cost%20of%20Delay%20Factsheets_Pennsylvania.pdf (accessed March 5, 2010).
Pew Center on the States. (2010b, February). The Cost of Delay: State Dental Policies Fail One in Five Children. Available at http://www.pewcenteronthestates.org/uploadedFiles/Cost_of_Delay_web.pdf (accessed March 5, 2010).
Pennsylvania Health Management Corporation. (2008). Public Health Management Corporation Household Health Survey Results. Community Health Database: An Information Service of PHMC. Available at http://www.chdbdata.org/datatool/surveyresults.asp (accessed April 2, 2010).
Reisine, S. T. (1988). The Impact of Dental Conditions on Social Functioning and the Quality of Life. Annual Review of Public Health, 9(1-19): 2.
Sheiham, A. (2006). Dental caries affects body weight, growth and quality of life in pre-school children. British Dental Journal, 201(10): 625.
St. Christopher’s Foundation for Children. (2010, March). Unpublished Care Mobile records, furnished by staff. Philadelphia.
U.S. Department of Health and Human Services. (2000). Oral Health in America: A Report of the Surgeon General—Executive Summary. Rockville, Md.: U.S. Department of Health and Human Services, National Institute of Dental and Craniofacial Research, National Institutes of Health. Available at http://www2.nidcr.nih.gov/sgr/execsumm.htm#execSumm.
Worldental.org. (2010, March 24). How Dental Care Will be Changed by Healthcare Reform. Dental Health Magazine. Available at http://worldental.org/dental-news/how-dental-care-will-be-changed-by-healthcare-reform/1209/ (accessed April 13, 2010).


